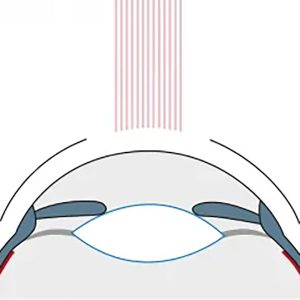
The cornea is the clear, front window of the eye. It helps focus light into the eye so that you can see. The cornea is made of layers of cells. These layers work together to protect your eye and provide clear vision.
Your cornea must be clear, smooth and healthy for good vision. If it is scarred, swollen, or damaged, light is not focused properly into the eye. As a result, your vision is blurry or you see glare.

If your cornea cannot be healed or repaired, your eye surgeon may recommend a corneal transplant. This is when the diseased cornea is replaced with a clear, healthy cornea from a human donor.
What Causes Cornea Problems?
Eye disease and injuries can damage the cornea. Here are some common eye problems that can lead to a damaged cornea:
- Keratoconus, where the cornea is cone shaped rather than dome-shaped
- Fuchs’ dystrophy, where cells in the inner layer of the cornea are not working effectively
- Eye infections or injuries that scar the cornea
- Previous corneal surgery or other eye surgery that damaged the cornea
Corneal Transplant Surgery Options
A human donor is someone who chooses to donate (give) his or her corneas after their death to people who need them. All donated corneas are carefully tested to make sure they are healthy and safe to use.
There are different types of corneal transplants. In some cases, only the front and middle layers of the cornea are replaced. In others, only the inner layer is removed. Sometimes, the entire cornea needs to be replaced.
Full thickness corneal transplant
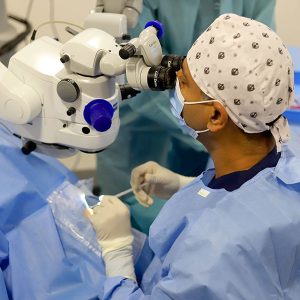
Your entire cornea may need to be replaced if both the front and inner corneal layers are damaged. This is called penetrating keratoplasty (PK), or full thickness corneal transplant. Your diseased or damaged cornea is removed. Then the clear donor cornea is sewn into place.
PK has a longer recovery period than other types of corneal transplants. Getting complete vision back after PK may take up to one year or longer.
With a PK, there is a slightly higher risk that the cornea will be rejected compared to other types of corneal transplants.


Partial thickness corneal transplant
Sometimes the front and middle layers of the cornea are damaged. In this case, only those layers are removed. The endothelial layer, or the thin back layer, is kept in place. This transplant is called deep anterior lamellar keratoplasty (DALK) or partial thickness corneal transplant. DALK is commonly used to treat keratoconus or bulging of the cornea.
Healing time after DALK is shorter than after a full corneal transplant. There is also less risk of having the new cornea rejected.

Endothelial keratoplasty
In some eye conditions, the innermost layer of the cornea called the “endothelium” is damaged. This causes the cornea to swell, affecting your vision. Endothelial keratoplasty is a surgery to replace this layer of the cornea with healthy donor tissue. It is known as a partial transplant since only this inner layer of tissue is replaced.
There are a few types of endothelial keratoplasty. They are known as:
- DSEK (or DSAEK) — Descemet's Stripping (Automated) Endothelial Keratoplasty
- DMEK — Descemet's Membrane Endothelial Keratoplasty
Each type removes damaged cells from an inner layer of the cornea called Descemet’s membrane. The damaged corneal layer is removed through a small incision. Then the new tissue is put in place. Just a few stitches—if any—are needed to close the incision. Much of the cornea is left untouched. This lowers the risk of having the new cornea cells being rejected after surgery.

What to Expect When You Have a Corneal Transplant
Days or weeks before your transplant
Your ophthalmologist will talk with you about corneal transplant surgery. You will discuss why you need this surgery, how it can help you see better, and what you can expect during and after surgery. Once you decide to have a corneal transplant, a date will be chosen for surgery. That date may change if a good donor cornea is not ready for you at that time. Tell your ophthalmologist about all the medicines you take. He or she will tell you if you can keep taking them before surgery.
You may need to stop using blood thinners before surgery. You may need to visit your primary care doctor for a physical exam and perhaps other tests. This is to make sure you are healthy enough to have the transplant surgery.
You will not be able to drive after the transplant surgery. You should make arrangements for someone to drive you home after surgery.
An opportunity for clear vision
If you have a damaged cornea, you and your ophthalmologist will discuss your options for improving your vision. For people with a deeply scarred or swollen cornea, transplant surgery can restore clear vision.
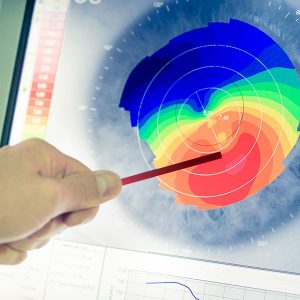
Your Personalised Procedure
To determine which procedure is right for you, a comprehensive assessment is conducted utilizing state-of-the-art technology. Based on the thorough diagnostic assessment, your surgeon will tailor a treatment plan to match the right procedure for your unique vision needs.